Medical Cannabis for Chronic Pain: What Patients and Research Are Saying
A growing body of patient data and clinical research suggests that many people with chronic pain report meaningful relief with medical cannabis, and a significant share reduce or stop certain prescription medications after starting it. The evidence is promising but uneven, and results vary by pain type, product, and individual. Here is what you actually need to know.
Chronic pain affects an estimated 51 million Americans. For many of them, prescription medications provide only partial relief, come with side effects, or carry long-term risks. That reality is driving a steady shift in how patients and physicians are thinking about medical cannabis.
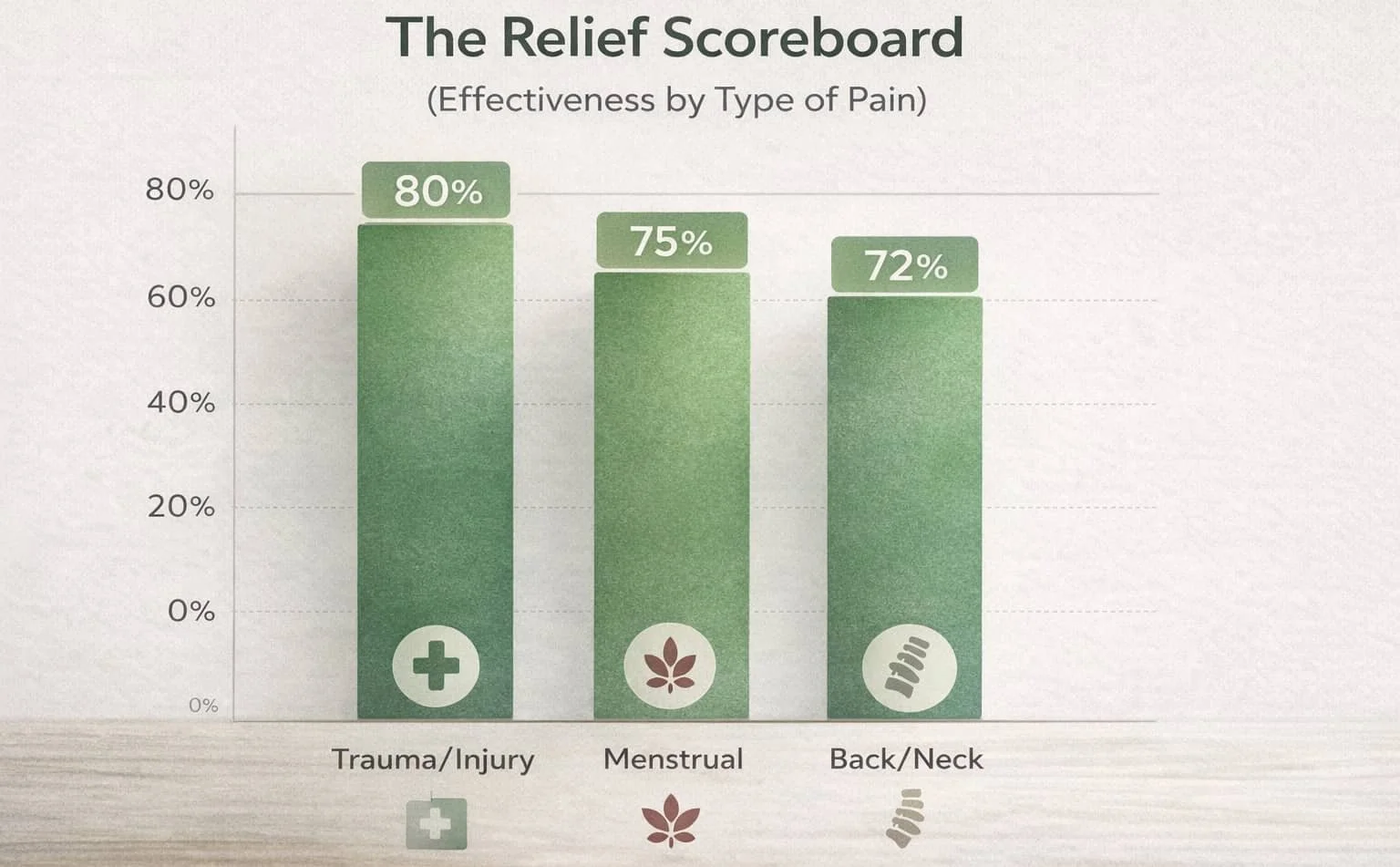
What did the 74.7% study actually find?
The figure comes from a peer-reviewed study published in the journal Cannabis examining patient-reported outcomes among people using medical cannabis for chronic pain. When asked how effective medical cannabis was in treating their symptoms or conditions, patients rated it an average of 74.7% effective on a scale from 0 (no relief) to 100 (complete relief), with ratings above 7 out of 10 across all pain types studied.
That is a self-reported outcome, not a clinical trial result, and it is important to read it that way. What it tells us is how patients actually experience the treatment, which is meaningful information even when it falls short of placebo-controlled proof.
Is medical cannabis effective for chronic pain?
The honest answer is: for many people, yes, with important caveats.
The National Academies of Sciences concluded there is "conclusive or substantial evidence" that cannabis is effective for the treatment of chronic pain in adults. That is a high bar for a federal body to clear, and it reflects the weight of accumulated research rather than one favorable study.
A 2024 living systematic review published by NCBI, which synthesized research on cannabis and plant-based treatments for chronic pain, found that THC has demonstrated analgesic properties, though its psychoactive effects and potential for use disorder may limit its suitability for some patients.
What the research shows most consistently is that cannabis tends to be more effective for neuropathic pain, pain related to trauma or injury, and pain accompanied by poor sleep and anxiety than for purely mechanical or post-surgical pain.
Related: Why Cannabis Companies Need Special Insurance
How does it compare to prescription pain medications?
This is the question most patients actually want answered. The picture is nuanced.
A meta-analysis found no statistically significant difference in pain relief between opioids and nabilone, a synthetic cannabinoid, suggesting that cannabinoids may be as effective as opioids for certain types of pain.
A 2025 survey of 1,450 medical cannabis patients managing chronic pain found that 72.4% rated cannabis 8 to 10 out of 10 for pain relief, and 35% stopped all prescription pain medications after starting cannabis, while 14.8% stopped some and 11.6% reduced dose or frequency.
For context, 18% of respondents in that same survey reported no change in prescription use. Cannabis is not a universal substitute, and it works differently for different people.
Why are chronic pain patients turning to cannabis?
Several practical reasons come up repeatedly in patient surveys.
Side effect profile is one of the most common. Patients who participated in medical cannabis pilot studies reported that it effectively substituted certain prescription medications while leading to fewer side effects than the drugs they had been taking.
Sleep and mood are another factor. Chronic pain rarely travels alone. Most patients deal with disrupted sleep, anxiety, and depression alongside their physical symptoms. Across studies examining cannabis-based medicines for chronic pain, almost all found benefit for sleep in some or most participants. When sleep improves, pain perception often improves with it.
And for some patients, the concern is long-term opioid use. Data from a Michigan dispensary survey found that use of medical cannabis was associated with a 64% decrease in opioid use among patients who had previously relied on prescription opioids for chronic pain.
What types of chronic pain respond best to medical cannabis?
Not all pain is the same, and the research reflects that.
Neuropathic pain has the strongest evidence base. This includes diabetic nerve pain, pain from multiple sclerosis, and chemotherapy-related neuropathy. Research suggests a higher reduction in opioid use among patients with neuropathic pain compared to those with non-neuropathic pain, which is consistent with the idea that cannabinoids modulate pain pathways differently than opioids, making them particularly relevant for nerve-related conditions.
Musculoskeletal pain, including arthritis and back pain, is one of the most common reasons patients seek medical cannabis. The belief that cannabis has analgesic and anti-inflammatory properties continues to attract patients with chronic musculoskeletal pain toward its use, and while clinical evidence is still catching up, patient-reported outcomes are consistently positive in this category.
Cancer-related pain and pain from serious illness has a longer track record with cannabinoids, and many oncology settings now include cannabis as part of a broader symptom management approach.
What does the research say about reducing opioid use?
This is one of the most actively studied questions in cannabis medicine, and the findings are generally encouraging with some important nuance.
In a survey of 2,897 cannabis patients who had used opioid-based pain medication, 97% reported using fewer opioids when also using cannabis, and 92% found the side effects more tolerable with cannabis than with opioids alone.
Some research suggests that states which legalized cannabis for medical purposes experienced reductions in opioid prescribing and opioid-related deaths, though other research examining longer time periods has found the relationship to be more complicated. The evidence is real but not settled, and responsible clinicians present both sides.
What is clear is that for individual patients, the combination of physician oversight, appropriate product selection, and gradual titration can support meaningful changes in how much and what kind of pain medication someone needs.
What should you know before starting medical cannabis for pain?
Product matters more than people expect. Research suggests that balanced THC to CBD formulations may offer pain relief with fewer psychoactive effects than high-THC products alone. The right ratio depends on the type of pain, the patient's tolerance, and other medications in use.
Route of administration affects everything. Inhaled cannabis acts faster but lasts a shorter time. Oral products take longer to work but provide more sustained effects. Topicals stay local. Each has a place depending on the situation.
Start low and go slow. This is the most consistent advice across clinical guidelines for new patients. THC sensitivity varies significantly between individuals, and many first-time negative experiences come from moving too fast on dosing.
Cannabis interacts with other medications. Anyone on blood thinners, certain antidepressants, or sedatives should discuss cannabis with a physician before starting. These are manageable interactions with proper oversight, but they are real.
It is not for everyone. People with a personal or family history of psychosis, those who are pregnant, or those with certain cardiovascular conditions should have a thorough conversation with a clinician before considering cannabis for pain.
Is medical cannabis legal for chronic pain in Virginia?
Yes. Chronic pain is among the qualifying conditions for medical cannabis in Virginia. A licensed physician can evaluate your situation and, if appropriate, provide a certification that allows you to purchase from a licensed Virginia dispensary.
The evaluation process is straightforward and can now be done via telehealth, which means you do not need to travel to a physical office to get started.
What is the bottom line?
Medical cannabis is not a guaranteed fix for chronic pain, and anyone who tells you otherwise is overselling it. What the evidence shows is that for a substantial portion of patients, it provides meaningful relief, supports sleep and mood, and helps some people reduce their reliance on other medications.
The best outcomes tend to come from working with a physician who can match the right product and approach to your specific type of pain, your current medications, and your overall health picture. That is what an individualized certification consultation is for.
If you are in Virginia and want to understand whether medical cannabis could be part of your pain management plan, our licensed physicians can walk you through the options honestly, without pressure.
This article is for informational purposes only and does not constitute medical advice. Medical cannabis is not appropriate for every person or condition. Talk to a licensed clinician to understand whether it may be suitable for your individual situation.
FAQs
-
For many patients it works, but not for everyone. The National Academies of Sciences reviewed hundreds of studies and concluded there is substantial evidence that cannabis is effective for chronic pain in adults. That said, results vary by pain type, product, and individual. Neuropathic and musculoskeletal pain tend to respond better than other types. The honest answer is: it is worth a real conversation with a physician, not a yes or no from the internet.
-
Some patients do reduce or stop certain prescriptions after starting medical cannabis, and studies support that this happens fairly often. But you should never stop a prescription on your own. The right approach is to work with a physician who can monitor the transition, adjust doses gradually, and flag any interactions. Cannabis and opioids, for example, can interact in ways that need oversight.
-
Not necessarily. A lot depends on the product. High-THC formulations are more likely to produce psychoactive effects, while balanced THC to CBD ratios or CBD-forward products are used specifically to minimize that feeling. Many patients use cannabis for pain in the evening or at night, which sidesteps the issue entirely. A physician can help match the right product and timing to your daily routine.
-
Chronic pain is a qualifying condition in Virginia. The process starts with a consultation with a licensed physician who reviews your medical history. If cannabis is appropriate for your situation, they issue a written certification. You then register with the Virginia Board of Pharmacy and can purchase from a licensed dispensary. The entire evaluation can be done via telehealth, so no office visit is required.
-
Long-term use is an active area of research. What the current evidence shows is that cannabis has a more favorable safety profile than long-term opioid use for most patients, particularly around overdose risk and physical dependence. That said, regular use does carry its own considerations, including tolerance development and, for some people, dependence. Anyone using cannabis long-term for a medical condition benefits from periodic check-ins with a physician rather than ongoing self-management.